
NMPA Usability Requirements for Medical Devices on the Chinese Market
What Manufacturers Need to Know
September 2025
Executive Summary
1The Role of the NMPA in the Usability Approval Process
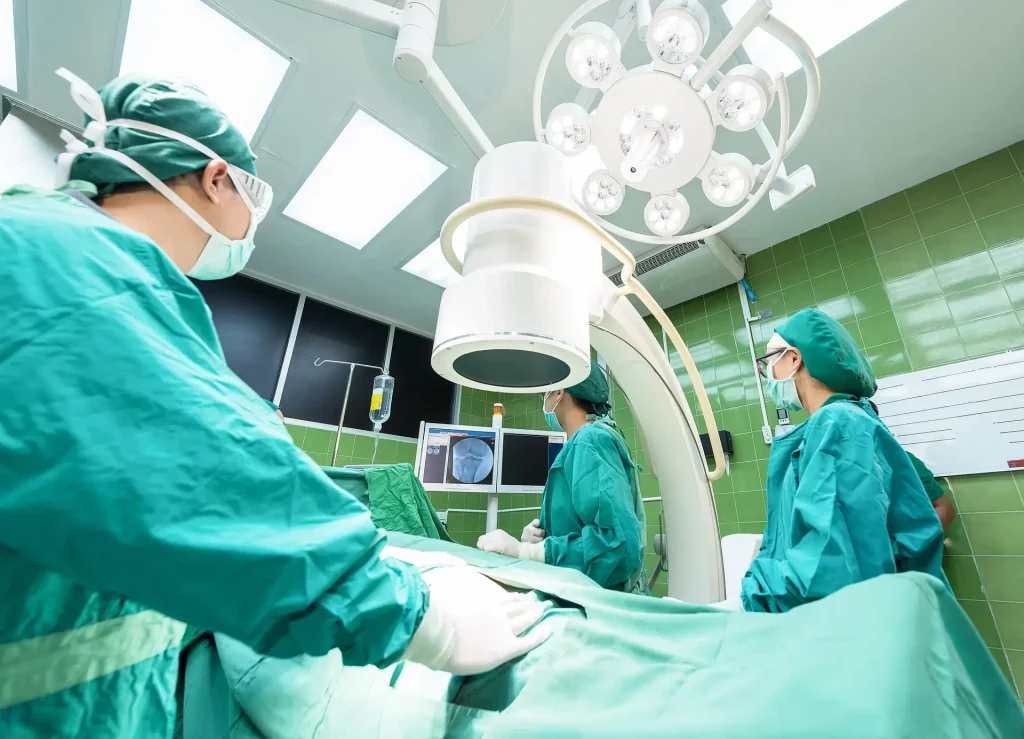
2Which Products Does the NMPA Usability Guideline Apply To?
Product Name
- Cardiac radio-frequency ablation equipment
- Cardiac radio-frequency ablation catheter
- Radio-frequency ablation equipment for cardiac surgery
- Radio-frequency ablation forceps/pen for cardiac surgery
- Surgical navigation and positioning system (with robotic arm and end effector)
- Endoscopic surgical system
- Control system for vascular interventional surgery
- Therapeutic ventilator
- Home healthcare environment ventilator
- External defibrillation equipment
- Haemodialysis equipment
- Continuous blood purification equipment
- Artificial liver device
- Implantable circulation assistance equipment
- Implantable drug infusion equipment
- Syringe pump (Class III)
- Needle-free injectors
- Infusion pump (Class III)
- Insulin pump (Class III)
Table: Product catalogue for high use‑risk products – according to the NMPA Guideline (as of October 2024)
3Scope of Usability Activities and Documentation
The extent of usability engineering activities expected by the NMPA primarily depends on the following aspects:
- The use‑risk level of the medical device
- The availability of comparable equivalent medical devices that are already available on the Chinese market
- The availability of human–machine interaction information for the identified equivalent medical devices
Depending on these variables, the NMPA expects the submission of one of the following two documents:
- Use error evaluation report
- Usability engineering research report
The following flowchart illustrates the recommended approach for determining the extent of usability engineering effort.
In the following, the individual steps are discussed in detail.
Step 1: Determination of the use‑risk level of the medical device
As an initial step, the use‑risk level of the product must be determined. In this context, the NMPA follows the established approach of both the FDA and IEC 62366‑1 by emphasizing that, due to the typically limited availability of data for risk classification, the focus should be placed on the severity of harm rather than on the probability of occurrence. In particular, the NMPA follows the approach of critical tasks, as already established by the FDA. In this regard, the NMPA defines the following:
- Incorrect use of Class II medical devices (medium use‑risk) may result in minor injuries.
- Incorrect use of Class III medical devices (high use‑risk) may result in serious injury or death. This concept is comparable to the FDA’s critical task approach.
- Completely new ways of use
- Long learning curves
- Use by lay users
- High operational complexity
- High use‑risk level: In the case of serious adverse events or Class I recalls related to use problems of similar medical devices after market launch.
- Medium use‑risk level: In the case of adverse events or Class II recalls related to use problems of similar medical devices after market launch.
- Low use‑risk level: If no adverse events have occurred, or only Class III recalls, or no recalls related to use problems of similar medical devices after market launch are present.
However, if a product with a High Use‑Risk level is present, an equivalent medical device comparative evaluation on the Chinese market must be conducted. For this purpose, a systematic search shall be performed to determine whether equivalent medical devices are already available on the Chinese market. Relevant sources include, in particular, NMPA registrations and publicly available product information.
Define clear criteria to justify equivalence. These may, for example, include the following aspects:
- alignment with respect to the intended use,
- alignment with respect to intended user profiles,
- alignment with respect to functional principles, and
- alignment with respect to characteristic user interface (UI) features (controls, displays, and labels),
in combination with equivalent user tasks and workflows.
4How are the Use Error Evaluation Report and the Usability Engineering Research Report structured?
Use Error Evaluation Report
- Basic information
- Level of risk of use
- Core elements
4a. Analysis of post-market use problems of similar medical devices
5a. Use-risk management
6a. Conclusion
Usability Engineering Research Report
- Basic information
- Level of risk of use
- Core elements
4b. Usability engineering process
5b. User interface requirements specification
6b. Use-risk management
7b. Verification and validation of the user interface
8b. User interface traceability analysis
9b. User training scheme
10b. Conclusion
Chapter 1: Basic information
Both documents begin with the basic information. The content is comparable to that of the use specification and primarily relates to general product descriptions. However, user profiles and the description of the use environment are to be provided in Chapter 3, “Core elements”.
Chapter 2: Level of risk of use
Chapter 3: Core elements
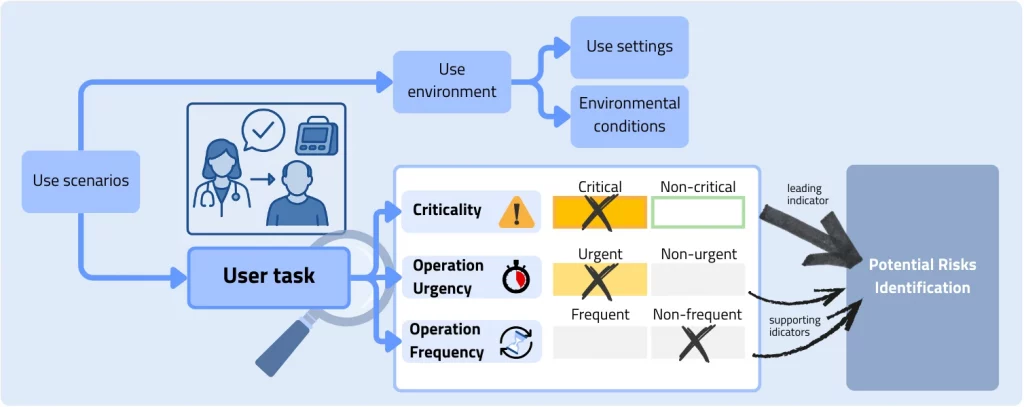
Practical examples for the general illustration of the classification of different user tasks
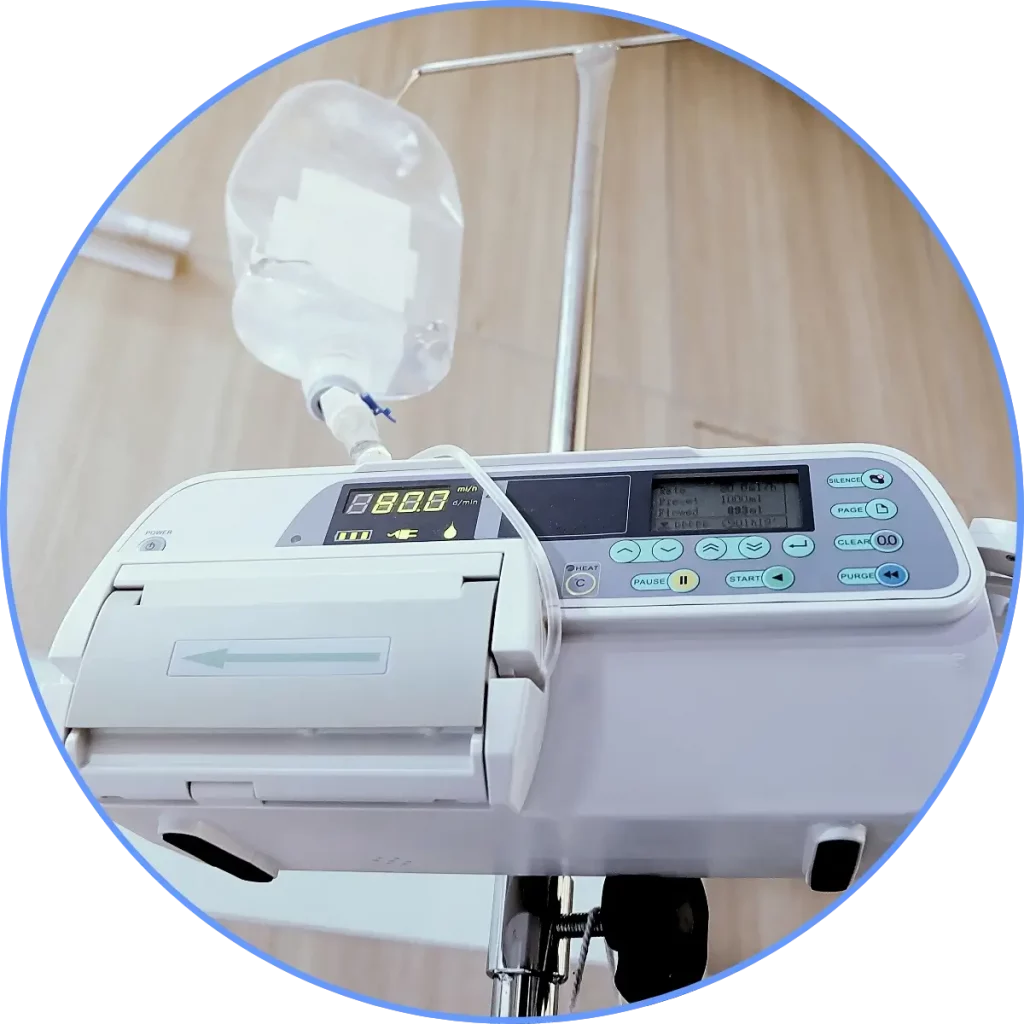
Setting the flow rate
- critical,
- non-urgent,
- non-frequent
Rationale:
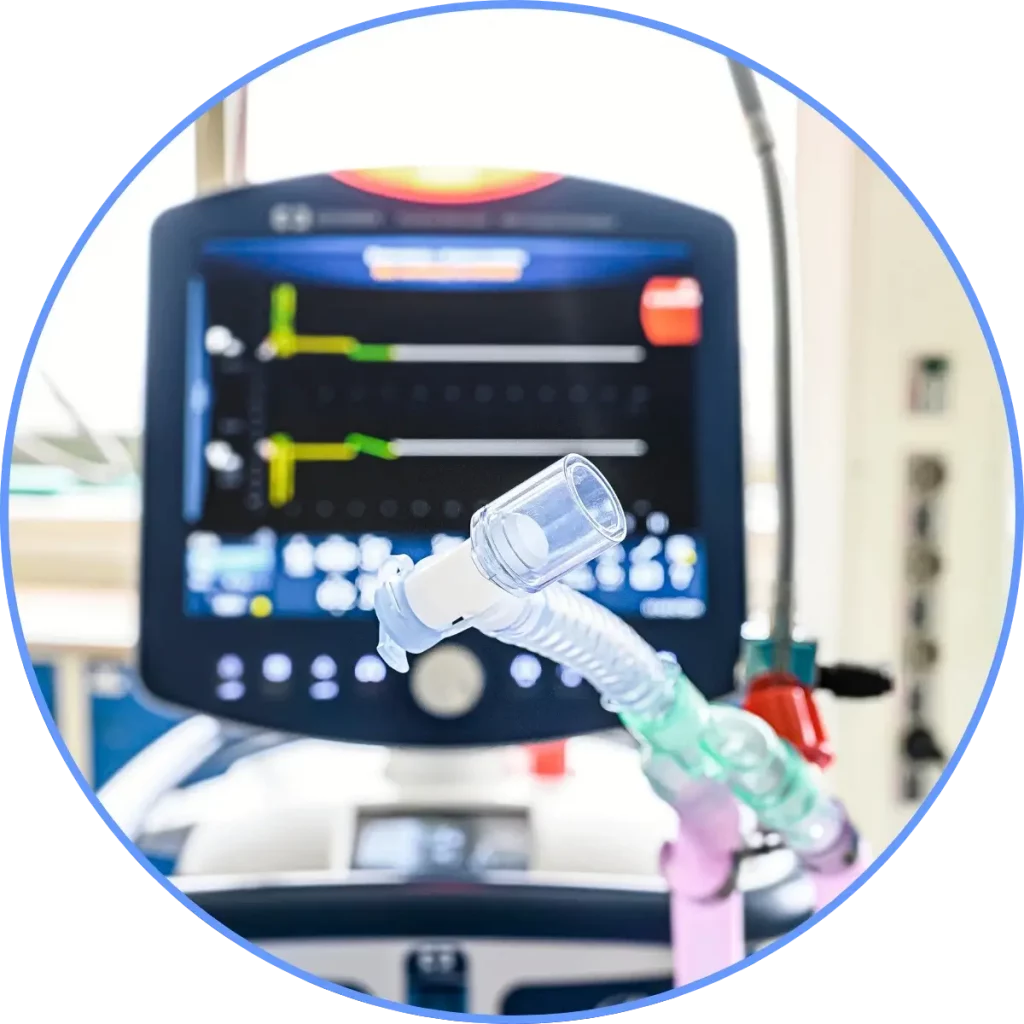
Ventilator
Immediate increase of oxygen concentration
- critical,
- urgent,
- non-frequent
Rationale:

Patient monitor
Confirmation of an alarm
- non-critical,
- non-urgent,
- frequent
Rationale:
Criticality – Confirmation of an alarm does not directly affect the patient’s physiological parameters. It serves system interaction rather than direct therapy adjustment. Potential harm arises only indirectly, for example through alarm fatigue or missed critical alarms. The task is therefore non‑critical.
Chapter 4a : Analysis of post-market use problems of similar medical devices
Chapter 4b : Usability engineering process
Chapter 5a & 6b: Use-risk management
Chapter 5b: User interface requirements specification
Chapter 7b: Verification and validation of the user interface
Chapter 8b: User interface traceability analysis
Chapter 8b, “User interface traceability analysis”, represents a novel requirement compared to other commonly used usability standards and guidelines. We recommend the development of a matrix structure that presents and cross‑references all previously described activities. This should be complemented by detailed descriptions of the relationships between the individual activities, explaining how the activities interact and interrelate.
Chapter 9b: User training scheme
If applicable, a training scheme for the medical device to be registered shall be developed at this point, describing the user training scheme, the materials, methods, and trainers used, and providing evidence of the evaluation of training effectiveness.
Chapter 6a & 10b: Conclusion
Here, the overall usability engineering process shall be briefly described in conclusion, essentially in the form of a management summary. In particular, it shall be demonstrated to what extent the use‑related residual risks have been reduced to an acceptable level, and that the safety and effectiveness of the user interface are ensured.
5When are usability tests required to be conducted in China?
Whether summative usability tests with the medical device are required is determined by the decision logic described in Chapter 3, “Scope of usability activities and documentation,” with the use‑risk level and the available data basis regarding equivalent medical devices being decisive. For products with high use‑risk and without robust evidence of an equivalent medical device, the NMPA generally expects a summative usability evaluation in the form of simulated use tests with Chinese users in a sufficiently simulated Chinese use context / simulation environment. The Guideline requires at least 15 Chinese participants per relevant user group in order to reliably identify use errors.
The Guideline provides for careful selection of participants, training where applicable, and data collection with a focus on the critical tasks. The Guideline emphasizes that individuals who frequently participate in usability tests of the same device or other devices from the same manufacturer should be excluded. Notably, compared to other guidelines, the NMPA Guideline explicitly expects a justification if no device training is required for test participants. The test reports should contain detailed information on the objectives, simulation conditions, results with respect to use errors and the associated root causes, as well as any deviations.
Once it has been determined that usability tests are required to be conducted in China, the question of practical implementation arises. While the NMPA does not specify a concrete qualification profile, it formulates clear requirements regarding the qualification and independence of the individuals conducting the tests – the evaluation shall be planned, conducted, and analyzed by individuals with demonstrable experience in usability testing of medical devices. Members of the manufacturing company who are heavily involved in the development of the device should not be assigned to conduct the evaluation.
- China‑specialized usability testing laboratories Conducting the study through partners with experienced usability testing personnel and their own infrastructure (laboratories, recruitment panels), with close substantive coordination with the manufacturer’s central usability team.
- Manufacturer‑internal implementation via local subsidiaries
Conducting the study at a Chinese subsidiary or in a company‑owned usability laboratory, provided that the moderating personnel are independent of the development team and have sufficient experience in usability testing; often in combination with external consulting to ensure NMPA‑compliant documentation.
6Conclusion – How to successfully prepare usability documentation for registration on the Chinese market
The “Guideline for Registration Review of Usability Engineering of Medical Devices” issued by the NMPA is the central reference for the assessment of usability within the Chinese registration procedure. For manufacturers with an established usability engineering process in accordance with IEC 62366‑1:2015, this means that the fundamental workflow—use specification, hazard-related use scenarios, formative and summative evaluations—remains familiar. However, the NMPA shifts the focus from a primarily internal usability engineering file toward reviewable documents that must stand on their own within the registration dossier (use error evaluation report or usability engineering research report). The recommended structure of these documents presented in Chapter 4 precisely reflects this dossier‑oriented approach.
For successful registration in China, it is therefore not sufficient to simply “submit” an existing IEC 62366‑1 process. What is decisive is that manufacturers consistently translate their usability evidence into the NMPA framework: with a clearly defined use‑risk level, a transparent decision logic (use error evaluation report vs. usability engineering research report), China‑specific summative usability tests where applicable, and reviewable documentation within the registration dossier. Manufacturers that proceed in such a systematic manner not only increase their chances of a timely market approval.
They also ensure that their products are used safely and effectively by the appropriate user groups in everyday clinical practice in China, in accordance with the labeling – thereby positioning themselves sustainably in one of the world’s most important MedTech markets.
Disclaimer
The information on standards and guidelines presented in this technical article has been prepared to the best of the author’s knowledge and expertise. It reflects solely the opinion of the author. No guarantee can be given with regard to the completeness, timeliness, or accuracy of the information provided. Standards and guidelines are subject to regular revisions and amendments, which may not always be immediately reflected here. This article does not constitute binding advice and does not replace a review of the applicable standards and guidelines by qualified experts or official bodies. For the application and interpretation of standards and guidelines, the currently valid original documents and the responsible organizations are authoritative.


